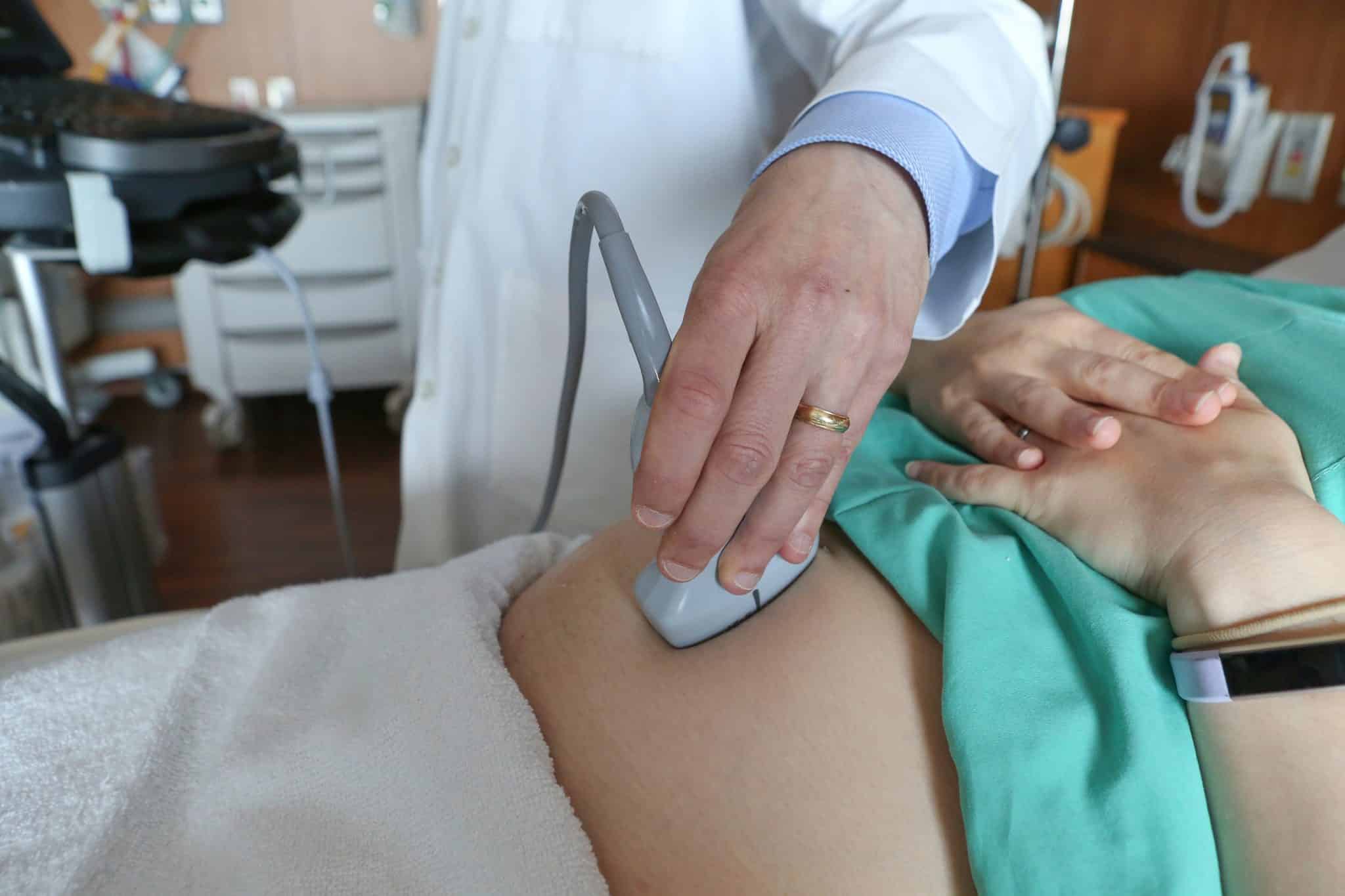
Early prenatal care improves the chances of having a healthy pregnancy and baby. But a new federal report shows it’s been on the decline. In Pennsylvania, late — or worse no prenatal care — increased from 2021 to 2024 by 7%.
The share of U.S. births to women who began prenatal care in the first trimester dropped from 78.3% in 2021 to 75.5% in 2024, according to data released recently by the Centers for Disease Control and Prevention (CDC).
Rachael Sampson, MD, Department of Obstetrics & Gynecology, Division of Maternal-Fetal Medicine with Capital Health Medical Center, spoke about what she is seeing in the county.
Dr. Sampson is a member of the Board of Directors for the Bucks County Medical Society. She came to Bucks County to practice full-scope women’s healthcare over 10 years ago. Even at that time, the landscape had already begun to change.
“A number of area hospitals had closed their labor and delivery units, leaving pregnant patients in Bucks County with fewer options,” said Dr. Sampson. “So, my patients had fewer options on where they were going to have this baby.”
Lower Bucks Hospital in Bristol closed their maternity unit in late 2012. The closure was the result of years of weak financial performance in the unit. This followed the departure of Lower Bucks’ busiest obstetrical practice, the Center for Woman’s Health in Langhorne.
The delivery hospital is the end point.
“That’s where the NICU is, that’s where it’s all at,” said Dr. Sampson. “The entry to prenatal care is so intricately linked to that labor and delivery floor. I can’t help but just think how it’s this loop, this cycle.”
Dr. Sampson was driven to complete fellowship training in maternal fetal medicine because she wanted to strengthen access to this subspecialty in Bucks County, “which is so intricately linked to that whole gamut, that whole nine months before you conceive, when you conceive, the entire prenatal care and then any of those potential complications that can occur during the course.”
She noted that labor and delivery is a very high-risk time. Dr. Sampson said these new CDC findings represent a shift because between 2016 and 2021, the timing of when U.S. women started prenatal care had been improving.
“In Bucks County, we know that for our county to flourish and for our communities to flourish, we need to support mothers and babies with high quality care before, during, and after pregnancy.” – Dr. Rachael Sampson, Bucks County Medical Society
CDC data indicated that early prenatal care (first-trimester initiation) in the U.S. improved from 77.1% in 2016 to a high of 78.3% in 2021.
So, then what happened?
Dr. Sampson said one potential confounder could be COVID.
“We don’t know what the impact of the coronavirus pandemic is,” said Dr. Sampson. “Some of our American College of Ob Gyn guidance in May of 2025 was to tailor prenatal care delivery for pregnant individuals. Coming out of the Coronavirus pandemic, there’s this idea that maybe care could be consolidated. Instead of having the traditional paradigm where you might get 14 prenatal visits, could that be accomplished in eight to nine high quality patient care encounters?”
Dr. Sampson thinks a lot of that is very attractive with everything that happened during Coronavirus. “Is there something coming off of that where patients are either distrustful of the medical system or of the traditional paradigm?” she asked.
A January 2025 KFF Tracking Poll on Health Information and Trust found the public’s trust in health information from key health agencies fell over the past 18 months, continuing a decline that began during the COVID-19 pandemic.
There are some advantages that they were able to harness during Coronavirus. “We were able to harness telemedicine, we were able to harness this concept of remote blood pressure monitoring, things that we haven’t completely figured out and that require technological costs and things that bounce off of that,” she said.
She said maybe there’s a reason why it translated into later care.
“The truth is that in order to have the best outcomes, you need to optimize medical conditions as early as possible,” said Dr. Sampson. “That’s what I find really concerning about any trend where patients are starting care later. You’re missing critical weeks where conditions could have been optimized; if that’s missed, that’s going to have downstream consequences.”
For example, the initiation of baby aspirin may be important.
“There’s key conditions where it makes sense to start baby aspirin and that has shown to decrease complications,” said Dr. Sampson. “That’s something that you really want to start early. You want to start that at 12 weeks. You want to have this needs assessment and these determinants picked up on well before 12 weeks.”
Having patients come in as early as possible receiving care and receiving touchpoint with a healthcare provider – that’s the way doctors are going to identify these things. Coming in later will affect their overall maternal health and mortality.
“The entire country has had a reduction in maternity care services and access to care nationwide.” – Dr. Mark Kuhn, who sees patients at Capital Health in Yardley and Langhorne
“We have hypertension on the rise,” said Dr. Sampson. “We have maternal cardiovascular disease, we have obstetric hemorrhage, embolism. Maternal health conditions are a top cause of maternal morbidity and mortality in this country. If you have screening factors, if you have touch points with healthcare providers, it’s only going to be beneficial because these are comorbidities that can worsen in the prenatal period.”
The postpartum period is another area.
“If it’s hard for patients to get in before they have the baby, imagine how hard it is after they have the baby,” she said. “If they’re getting care later and later and they don’t have an established care before they have the baby, where does that lead them once there’s a newborn and if the mom has critical complications?”
Insurance coverage or gaps in insurance and maternity deserts are always issues in health care.
The so-called “Big Beautiful Bill” cut $1.1 trillion from Medicaid and ACA marketplaces, according to Congressional Budget Office (CBO) estimates. Cuts include a provision that takes away Medicaid from people who are eligible for the ACA Medicaid expansion but can’t show that they meet a work requirement, red tape that blocks people from enrolling in health coverage they are eligible for, and provisions that take away health coverage from most categories of immigrants living lawfully in the U.S.
“Insurance coverage gaps are a concern for patients and providers,” said Dr. Sampson. “Access to care is crucial in order to optimize maternal health outcomes, along the lines with national trends that we’ve also seen in Bucks County where institutions that previously had labor and delivery services and by extension prenatal care services those no longer provide this. That is a concern.”
Dr. Sampson has worked on national and state committees and that’s helped her to highlight that their experience in Bucks County is in line with the national desire to provide safe childhood initiatives across this country. “In Bucks County, we know that for our county to flourish and for our communities to flourish, we need to support mothers and babies with high quality care before, during, and after pregnancy,” she concluded.
Dr. Mark Kuhn is a board-certified obstetrician and gynecologist who has provided women’s health services to patients in Bucks and Mercer Counties for nearly 40 years.
Dr. Kuhn currently sees patients at Capital Health in Yardley and Langhorne. He’s seeing patients coming in later in their pregnancies for prenatal care and more complicated patients.
“I’ve seen the sickest patients in my entire 40-year career in the last 15 years,” he said. Is it disparities in healthcare, social determinants of health, zip code? All of the same. But it certainly isn’t helped if people don’t come in for prenatal care. The earlier we see them, the more we can assess different problems and enhance their health.”
Dr. Kuhn said they see women from some areas and some socioeconomic groups coming in later for prenatal care.
“We see them coming in later for all sorts of different care,” he said. “The longer you wait with potential health problems, the more fraught with complications they can be. Maternal mortality is linked to complications of pregnancy, like hypertension, which can happen with a higher frequency in certain demographic groups, certain socioeconomic groups. And to the degree that those people come in later in pregnancy, their hypertensive problems are worse.”
He said in the vast majority of cases, it does not result in mortality. “But morbidity, which is the other side of that coin, is just overall sickness,” Dr. Kuhn said. “And that’s just not good for anybody nor for the healthcare system.”
There are differences in accepting insurance because of state requirements.
“We do see patients for prenatal care in Pennsylvania, but they end up delivering in New Jersey,” Dr. Kuhn said. “I don’t know how that is reflected in people who have Pennsylvania state sponsored insurance delivering in New Jersey. I don’t think they’re allowed to.”
“We used to practice at Lower Bucks Hospital in Bristol, which we loved, but they just got beat up and they had to close their labor and delivery unit,” Dr. Kuhn added. “The entire country has had a reduction in maternity care services and access to care nationwide.”
This article was made possible thanks to the Associated Press’ “Localize It” resources.